What Is Lymphedema?
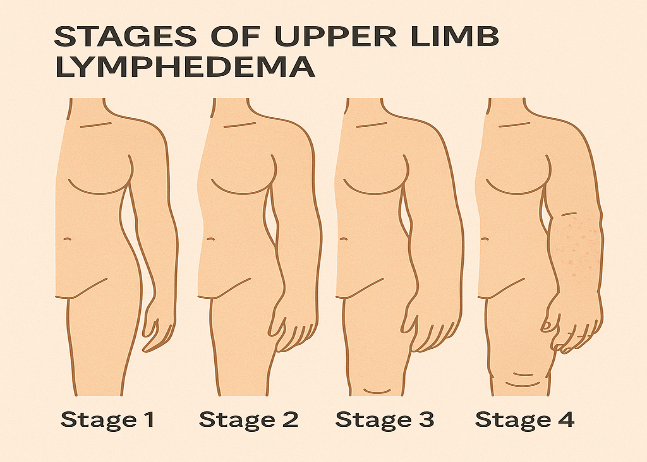
Lymphedema is a chronic condition that is caused by a disruption or damage to the normal drainage pattern in the lymphatic system. It most often causes swelling of the arm, but it can also affect the breast. The swelling, caused by an abnormal collection of too much fluid, is called lymphedema.
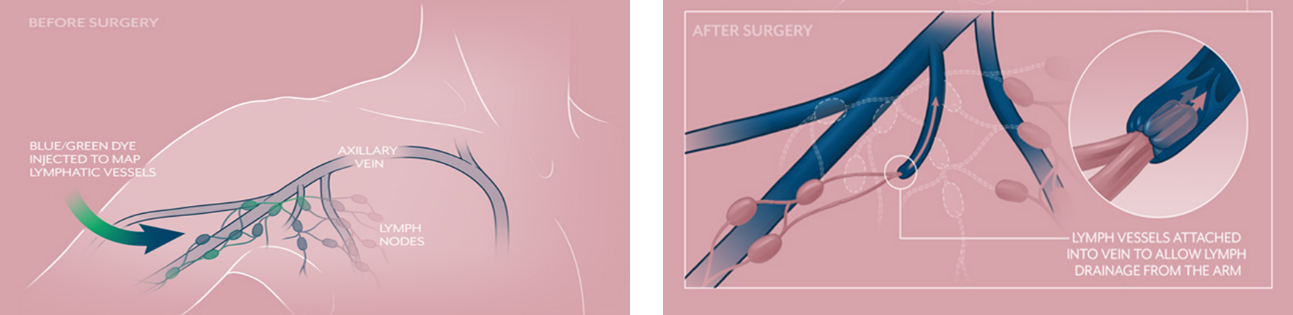
The underlying cause of lymphedema is multi-factorial. Removing the axillary lymph nodes increases your risk for developing lymphedema, because some lymph nodes in the axilla drain the lymphatic fluid from both the breast and the arm.The risk of developing lymphedema is related to the number of nodes removed and the number of treatment modalities provided to the axilla. After sentinel node biopsy only, the risk of upper limp lymphedema is 0-7%, and it increased to 20% after axillary node dissection. Receiving axillary radiation after surgery further increased the risk that may reach up to 40%, owing to additional damage to the lymphatic system in the axilla. Certain types of chemotherapy agents are associated with increased risk of lymphedema as well.